How to use data for everyday decisions in a pandemic

With the end of widespread lockdowns, and as the wait for a vaccine to become widely available continues, the onus is on us as individuals to take precautions and decide on safe actions.
Research on what activities are classified as being ‘safer’ and country guidelines are a helpful starting point, but these are insufficient. Not all situations are documented, and there is significant contextual variation making a “one-size-fits-all” approach infeasible.
Thus, individuals are left to assess the risks and make safe decisions for every activity, whether it be stepping out to the neighborhood café for a cup of coffee, inviting people home to a child’s birthday party, or resuming work in an office space.
To arrive at an answer for each such instance, one should systematically evaluate the circumstances with evidence and data, and use it to address the worrying questions on one’s mind, “Will I get infected? If I do, will I transmit to others? Will I need hospitalization?”
Personal anecdotes, political rhetoric, and sensational media stories reinforce cognitive biases, which may lead to extreme behaviors. Some people may continue to remain at home, as if still in lockdown, in anticipation of spikes in cases and disturbing stories of an overburdened health care system. Others might resume their lives and engage in activities as if the crisis had abated and normalcy was restored.
In order to adopt a fact-based approach to decisions that can help overcome biases, the right data needs to be made available from reliable sources and in a timely manner, such that it allows combining data from different sources for meaningful analysis and interpretation.
A holistic approach to using data for decision-making
J-PAL South Asia’s Innovations in Data and Experiments for Action (IDEA) Lab collaborates with governments, nonprofits, and private data providers to enable greater use of data for decisions by engaging in data use cases and strengthening capabilities to improve quality and use of data for decisions.
Many governments, including in large countries like India, where J-PAL South Asia is based, have deployed digital technologies such as app-based data collection and monitoring technologies in the fight against the pandemic. With the expansion of digitization, data on tests, cases, deaths, and recoveries is publicly available daily in almost real time.
Such data is frequently used to describe current and past trends, but is under-utilized for forward planning and decision making.
A framework for decision-making
For a starting point in the use of data for decisions, one can adopt the principles of a decision framework, which is both a conceptual structure and a way of processing all pertinent information objectively to inform the best course of action given the circumstances.
For decisions at any level, whether an individual, business, or government, there are three natural steps in a data-driven process:
(i) Defining estimating indicators,
(ii) Identifying data sources, and
(iii) Combining data to appropriately estimate and interpret indicators.
In this post, we’ll discuss the decision framework from the point of view of individuals making decisions on undertaking day-to-day activities such as going to a cafe, a salon, or shopping in a mall.
Defining indicators
The first step in developing a decision framework is to identify the right indicators.
Indicators are contextually valid metrics that allow us to assess a particular situation. Country or state-level number of cases, deaths, and recoveries are the most commonly used indicators to understand the general trend of the pandemic, but may not be relevant to assess the situation locally in a given neighborhood.
We outline a few indicators below which we believe will help us as individuals assess the local situation and inform personal decisions.
First, we need an indicator for personal risk profile: What percentage of people with similar characteristics, in terms of age, gender, and co-morbid conditions get infected and experience adverse effects of the disease?
We have to estimate this not just for ourselves as individuals (personal risk), but also for those we live with (household risk), since if we get infected when we venture outside, we endanger them as well. This can be estimated using national data on testing, symptoms, behavior, hospitalization, and deaths for persons with similar characteristics to us and our household members.
Next, we need an indicator to assess the health system response of our city: If we or anyone in our homes are infected, how quickly and effectively can the city’s infrastructure respond to a need for hospitalization?
Typically, this indicator includes the time taken between clinical recommendation and actual hospitalization (average time taken for hospitalization and treatment), availability of resources, such as beds, and the receipt of the prescribed care protocol (prescribed medication, oxygen support, or ICU care). To estimate this, city-level data on time to hospitalization, quality of treatment, and availability of hospital resources such as oxygen supply and ICU can be used.
Then, we need an indicator to understand the local situation: How prevalent is the disease in our neighborhoods?
For example, how many people on an average out of, say, 10,000 residents are infected? Have the cases increased or decreased over the past few weeks? This is estimated using neighborhood-level data on cases to estimate prevalence.
Since research suggests that the likelihood of contracting the virus varies in different situations, we need an indicator for disease transmission: In what percentage of cases can the source of infection be linked to places of sustained exposure (household, offices, etc.) or sporadic exposure (restaurants and commercial establishments)?
Similarly to prevalence, neighborhood-level data is useful to estimate the likely source of infection.
Indicators represented as percentages, indices, or scales, rather than absolute numbers, are more helpful since they help compare across situations.
In order to use indicators for a decision, we must estimate value by using reliable data from the right levels.
Combining data sources to estimate indicators
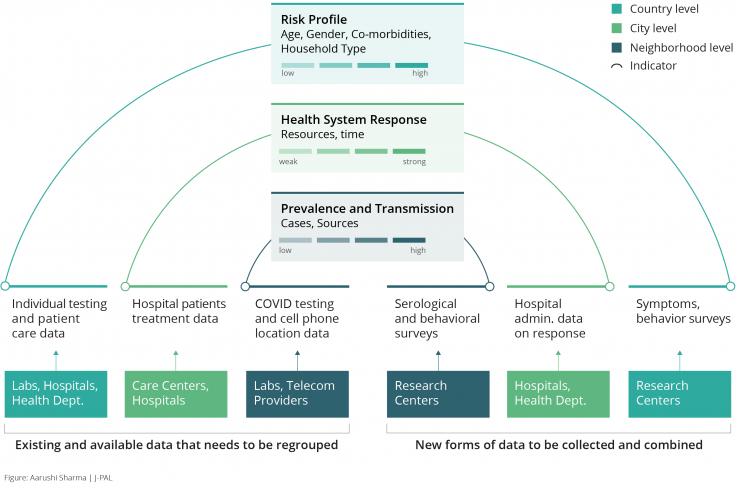
While the framework represented above serves as a thought exercise, it can be operationalized when the right data is available, and when there is potential to collect and combine more data through various sources (see Figure 1).
Several such initiatives are already underway, albeit in silos. For instance, all public and private testing labs in India report on tests and outcomes they carry out; and hospitals, isolation centers, and home isolation monitoring programs keep detailed clinical records on disease progression, treatment, symptoms, and recovery. If collated centrally, this data could be used to estimate individual localized indicators for prevalence and risk profiles.
In addition, central and state government apps in India like Arogya Setu compile information on positive cases, movement of users, and hotspots. Cell phone location data captures information on the movement of users and interaction by location, type of business, and time of day. Such data, in addition to data from serological (antibody) surveys, can be combined to provide estimates of local transmission by type of business and activity.
Household surveys, such as the one conducted in West Bengal by J-PAL affiliated researchers, can provide information on symptoms and health-seeking behavior, adding more nuance to the estimation of risk profiles.
Administrative data on hospital beds and ICU facilities and real-time data on emergency services can be collected and collated from all institutions providing treatment in the city and used to estimate the health system response.
Finally, all the data should be anonymized and organized such that it lends towards group-wise estimation by personal characteristics, community, and city.
Applying the framework
Once we have determined what types of indicators to assess, what statistics each indicator consists of, and where to source the data from, it is possible to use such a decision framework for different individuals in different locations to decide how risky it may be to engage in a local activity such as going to a cafe in their neighborhoods and cities (see Figure 2 for an example of two scenarios).
This type of analysis is more personalized and informative than general guidelines, as people are resuming their lives and activities and may not consider more general guidelines to apply to them.
This example showcases these indicators for two similar people in different cities with comparable health systems/responses, different household composition, facing different prevalence rates in their respective neighborhoods.
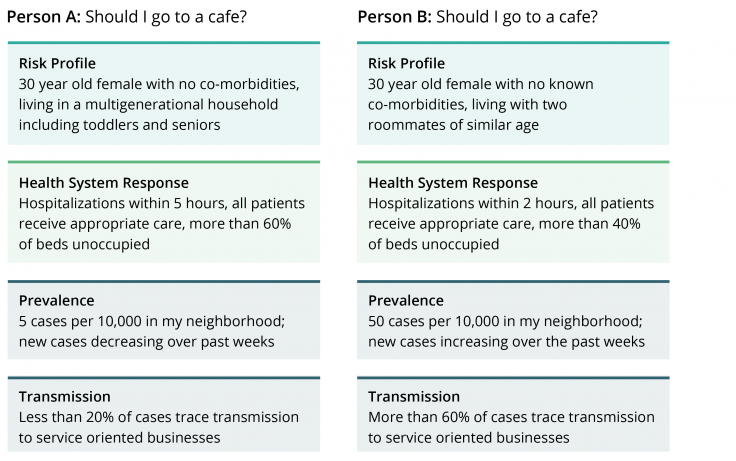
As we can see, the assessment of the riskiness of the activity varies, based on the estimation of each indicator using data from their respective situations.
The final decision should be informed by a cost-benefit analysis: a comparison of the computed risk based on one’s personal and household profiles and type and location of activity, to the perceived benefit from the act of, in our example, visiting a cafe.
Today, app-based solutions, like an indicator dashboard that’s updated in real-time, could easily compute conditional probabilities and statistical modeling. We’ve mocked up an example of what this might look like in Figure 3, though it remains just a concept for now.
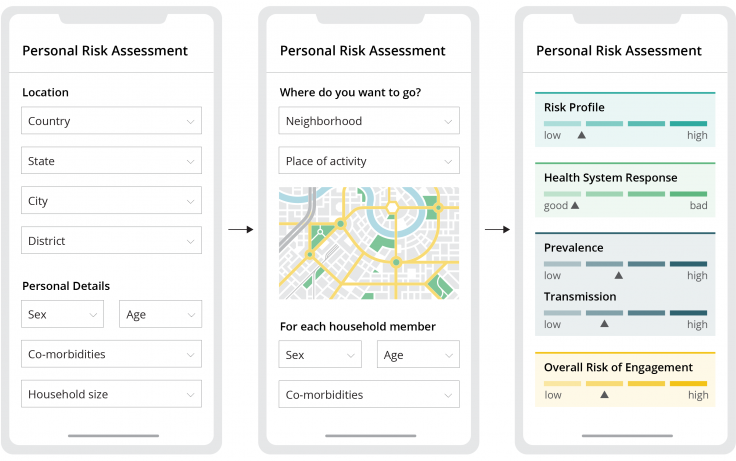
Expanding beyond personal decision-making
Such apps are meaningful only if all relevant data from different sources are accessible and collated for ease of use, while ensuring appropriate data protection features.
The success of such an initiative eventually depends on its use. There is an urgent need for governments to involve citizens, researchers, and industry leaders in the safe and effective use of data for decisions.
However, even with the right data on smart dashboards at our fingertips, what ultimately matters is nurturing the habit of a data-driven approach to thinking across levels, by individuals and within organizations and governments to reduce our biases and make better decisions.
To enable effective data use over time, much more needs to be done on policies for the protection of sensitive information, guidelines, and protocols for data accessibility and feedback mechanisms into policy decisions. J-PAL's IDEA Handbook on Using Administrative Data serves as a go-to reference, providing rich information, best practices, and case studies of collaborations between data providers and researchers.
To start with, data use cases, i.e. instances of combining and interpreting data for insights into planning and course correction of policy actions, can effectively demonstrate how data can be a decision-making tool. The authors are presently working on a proof-of-concept dashboard to demonstrate this decision framework using publicly available data.
With real-time data, the application of the model could be expanded to inform a wide range of decisions. For example, a city government interested in developing a technical platform could partner with J-PAL’s IDEA Lab to define the right indicators and data sources into a decision framework, operationalize the use of data for decisions such as the opening of schools and running of businesses operations.
Finally, such platforms would enable policymakers to engage with researchers to design and evaluate the impact of a variety of interventions to enable safe resumption of social and economic activities, truly unlocking the potential for innovative use of data for decisions.
Harini Kannan is a research scientist at J-PAL South Asia who focused on research in education and providing M&E advisory to state governments, NGOs, and other social sector organizations.
Aparna Krishnan leads the IDEA Lab at J-PAL South Asia and works with governments on institutionalizing the use of evidence to inform policymaking.
Using de-identified location data captured in smartphones, researchers worked with J-PAL Southeast Asia to study movement patterns to analyze how Indonesians changed their behaviors during the initial phases of COVID-19 and during the lockdown.
Many policymakers are concerned about the costs of suspending economic activity due to COVID-19 lockdowns. Several have argued that enforcement of lockdowns will adversely affect the most vulnerable groups who do not have savings and rely on the informal sectors.
With this in mind, it’s useful to more clearly determine whether economic losses are caused by the enforcement of lockdowns, or rather by people’s own behavior in response to COVID-19. In other words, did people become less mobile as a result of the formal government-sanctioned lockdown, or as a result of the pandemic itself?
Indonesia provides a useful case study to answer this question, as lockdowns have been enacted in a decentralized and gradual way.
Several provinces adopted lockdowns or what was called "large-scale social restrictions" (Pembatasan Sosial Skala Besar, or PSBB) in Indonesia gradually by submitting requests to the Ministry of Health. For example, Jakarta applied for PSBB on April 2, and its PSBB was approved and started on April 10; while several other regions were initially rejected based on the number of cases in those areas.
To further manage the spread throughout Indonesia, long-distance train and air travel were also shut down at various dates in April, preventing Mudik, an annual tradition when millions of families travel to home villages near the end of Ramadan.
Using de-identified location data captured in smartphones obtained from the company Veraset, we worked with J-PAL Southeast Asia to study movement patterns to analyze how Indonesians changed their behaviors during the initial phases of COVID-19 and during the lockdown.
This data helps us understand mobility patterns, such as same-day commuting and inter-regional travel, as an indirect measure of economic activity—for example, commuting to the office, going shopping, and conducting trade activities.
Smartphone location data showed big changes in people’s mobility
The study found many smartphone users changed their behavior abruptly by reducing mobility when the number of COVID-19 cases begins to rise, followed by low and further decreasing mobility afterward. People made a one-time adjustment away from urban areas to other districts in late March, and the rate of inter-district travel remain small with a further decrease thereafter. Lastly, mobility was already low and changed little when the formal PSBB restrictions were implemented in Indonesia's major cities.
The analysis used location information from almost 60 million smartphone users in Indonesia for at least one point in time from January until May 2020. We restrict the sample to a smaller set of users who can be observed regularly during the timeframe.
This sample has some characteristics that may not reflect the larger population: Since the data only contains information from smartphone users, one could assume that they are likely to have a higher income than non-smartphone users. Migrant workers are 15 percentage points more likely to use smartphones than non-migrants who have the same level of household expenditure, so they are over-represented in this data. Nevertheless, in urban areas in Indonesia, smartphone use is already high. In the Jakarta capital region, it is 62 percent, 56 percent in predominantly urban districts, and 42 percent overall.
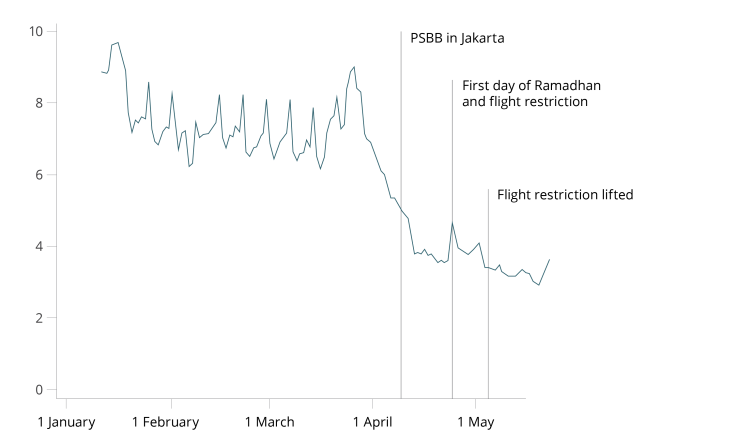
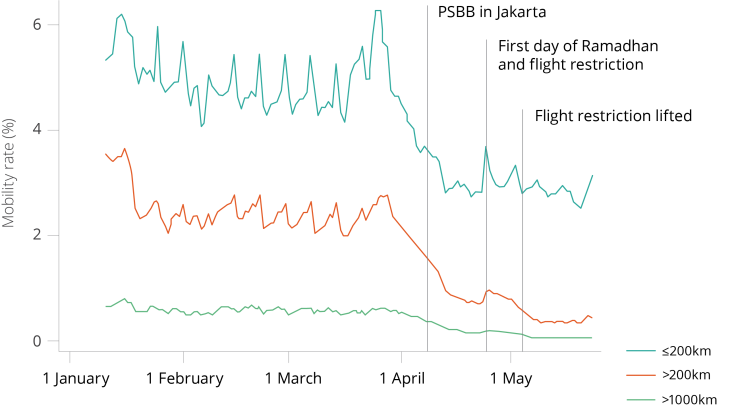
People stayed at home following the President's call to reduce COVID-19 transmission
To understand the changes in the rate of commuting and daily trips made by users, we measure same-day movement by comparing where users are during the night compared to daytime hours.
In January-February, before COVID-19 cases began to rise in Indonesia, the fraction of people staying home (defined as no travel beyond 200m away from nighttime location) on a given day ranges around 50 percent in Jakarta to 60 percent on average nationwide. After the President of Indonesia's speech on March 15 highlighting the urgency of COVID-19 and the call for social distancing, and as many other countries were introducing formal lockdowns, the fraction of people staying at home started to grow.
Two weeks later, the rate reaches around 80 percent and stays there until late May, at least. This is supported by the closing of schools and offices beginning to implement work-from-home policies. During national holidays, i.e., Indonesian Labor Day, Eid al-Fitr, the rate of people staying at home decreased further, with almost 90 percent of users remaining at home.
When the formal PSBB (lockdown) was introduced, Jakarta was the first region to implement the restriction on April 10, and the rate of mobility was already low. There was no noticeable jump in the number of people staying at home both in Jakarta and nationwide.
This suggests the changes in economic activity driven by smartphone users commuting to workplaces, traveling to shopping centers, or traveling for other purposes has already taken place, and were not a result of the formal lockdown.
People moved, then stayed, to adjust to lockdowns
We also looked at inter-district travel to understand changes in commuting and other daily economic and social activities, such as business travel, migrant workers traveling for work, and family travel. We analyzed medium- and long-distance travel between 500 districts in Indonesia by determining the median nighttime location for each user and defining that a user has moved if on a given night, they are found to be in a different district than two weeks prior.
At the start of the year, we observed a regular spike of weekend travel among users in and out of districts. After March 15, there is a large net outflow away from cities that lasts approximately two weeks. The travel flow then falls to around 50-75 percent compared to January-February.
The rate of travel remains low over the five months of observation, though an exception occurred at the start of Ramadan (concurrent with days leading to the ban of most internal passenger air travel). The small spike in travel happened in the context of "mudik," the Indonesia yearly return of migrants to their hometown at the end of Ramadan.
In anticipation of travel restrictions due to lockdowns, many migrant workers may have preemptively left large cities to avoid getting stuck. Due to the lack of nationwide lockdown and instead gradual regional restrictions, migrants who wanted to leave had the time to return to home regions.
Policy Takeaways
- Fear of COVID-19 played an essential role in the changes of people's mobility patterns. Results from this analysis show that people were sensitive to the information and recommendations provided by governments. Even without the formal lockdown of most economic activity, people could understand the urgency of the situation to limit the spread of the virus.
As countries begin to reopen its economy and adapt to the pandemic, it is worth noting that a false sense of familiarity with the virus may attenuate the initial fear despite the increasing rate of COVID-19 cases. This may further increase the COVID-19 trajectory of cases, leaving a share of the population from returning to their previous level of activity and impacting the economy. - Migrants anticipate formal restrictions that may trap them, and may travel due to the sudden decrease in job prospects in cities. However, after months of staying at home, many households may no longer be able to prioritize health concerns over their economic needs. This may be especially true for low-income workers who may be under-represented in our data.
- With or without active government lockdowns, the results strengthen the case for active government support to people affected by the economic disruption. Our analysis shows some economic loss driven by mobility is not necessarily led by formal government lockdowns and is influenced by how people react to the pandemic. To face the economic loss experienced by families indirectly caused by COVID-19, government should expand its social protection policies to reach vulnerable people as part of every country's COVID-19 strategy (Hanna and Olken in EPoD).
For more, see the original op-ed "Lockdown and Mobility in Indonesia" in the Centre for History and Economics.
Better understanding and addressing the social determinants of health is critical to improving individual and population health and advancing health equity. J-PAL North America’s COVID-19 Recovery and Resilience Initiative aims to contribute to knowledge in this area by testing strategies to minimize the short and long-term public health impacts of COVID-19 and address inequities in access and care.
The COVID-19 pandemic has placed unprecedented strain on the American healthcare system, and in doing so has brought to light many of its most persistent shortcomings. Despite spending far more than any other country on healthcare, the United States has reported the highest number of coronavirus cases and the highest number of related deaths, causing many to question the underlying structures of the nation’s health care system. Gaps in health care access, coverage, and quality based on race, socioeconomic status, and geographic location are, in the midst of a global pandemic, rapidly widening and becoming more apparent than ever.
As nationwide protests against police violence and systemic racism continue across the United States, blatant disparities in COVID-19 infections and deaths point to the pressing need to address inequities in health and a myriad of other areas. Narrowing the significant socioeconomic gaps in health care access during the pandemic and post-pandemic context is an imperative undertaking.
Better understanding and addressing the social determinants of health is critical to improving individual and population health and advancing health equity; without taking an intersectional approach to addressing health, disparities will persist and communities will be left behind in the fight to mitigate the impact of COVID-19 and recover from the pandemic.
J-PAL North America’s COVID-19 Recovery and Resilience Initiative aims to contribute to knowledge in this area by testing strategies to minimize the short and long-term public health impacts of COVID-19 and address inequities in access and care. By teaching policymakers what programs and policies work to improve health equity and access, rigorous evidence can play a fundamental role in helping the nation respond effectively to COVID-19 while building a more equitable healthcare system in the long-run.
Pre-existing inequity in health care delivery and access
Communities of color have been hit the hardest by the COVID-19 pandemic, reflected in higher infection and death rates for Black, Hispanic, and Indigenous populations. These disparities in COVID-19 diagnoses and deaths are the result of pre-pandemic realities that have long limited access to health care and wealth. Structural factors—such as residential segregation and gentrification, workplace conditions, and economic security—have worked to reinforce and intensify health disparities by socioeconomic status, and contributed to rates of pre-existing health conditions that correlate with higher vulnerability to COVID-19.
Additionally, Black, Hispanic, and Indigenous communities in the United States often have less access to quality health care: even before the arrival of the novel coronavirus they were significantly more likely to be un- or under-insured. Immigrant communities are especially likely to be uninsured, as they are overrepresented in jobs that do not provide health insurance coverage, and undocumented individuals are explicitly barred from accessing most public and employer-sponsored plans.
There is also a history of distrust between these communities and the American health care system stemming from inaccessible care, disparities in health outcomes, a lack of Black, Hispanic and Indigenous physicians, and, for Black Americans, a longstanding history of medical exploitation and abuses dating to slavery.
Contact tracing, a public health tool that asks individuals to divulge personal, detailed information, inherently requires a degree of trust that our healthcare system has failed to earn from many communities of color. The combination of systemic distrust coupled with disparities in the quality of housing, jobs, and care available to communities of color has resulted in disastrous health outcomes for Black, Hispanic, and Indigenous communities during the COVID-19 crisis.
The impact of COVID-19
Amidst a global health crisis that has had catastrophic impacts on public health globally, the United States’ healthcare system has been hit particularly hard: the country has 4 percent of the world’s population, but about 24 percent of its COVID-19 cases and 22 percent of its COVID-19 deaths (as of September 1).
Overburdened hospitals serving the most hard-hit regions are struggling to pay for critical health services amidst rising equipment costs and declining revenues. They are also less able to provide quality primary care, mental health care, and care for chronic conditions in the struggle to funnel resources toward responding to COVID-19.
Deaths from noncommunicable diseases such as heart disease and diabetes have increased during the pandemic, possibly because individuals are afraid to seek emergency care out of fear of being exposed to the virus. On top of this, the United States is facing an unprecedented mental health crisis, with people experiencing higher rates of depression, anxiety, substance use, and suicidal ideation due to coping with the pandemic.
Nationally, Black and Hispanic populations have been disproportionately impacted by the virus, accounting for higher rates of infection and death than would be expected given their share of the national population. Of the 20 counties in the United States that have the highest level of COVID-19 deaths per capita, 11 counties have populations in which Black, Hispanic, or Indigenous people represent the largest racial group.
Adjusting for age, the coronavirus death rate for Hispanic populations is 2.5 that of white populations. For Black communities the numbers are even more harrowing, with Black populations dying at a rate of 3.6 times that of white populations. Part of the reason behind such disproportionate rates of infection and mortality stems from the fact that Black workers, Hispanic workers, immigrants, and women are disproportionately represented in essential, frontline jobs which dramatically increase one’s risk of exposure to the virus.
The economic impacts of the COVID-19 pandemic have had disastrous impacts on health inequities as well: the number of Americans living without health insurance has nearly doubled in size since late February, and families who have been financially impacted by the virus are struggling to pay for basic care. A disproportionate number of those losing employer-based coverage have been Black and Hispanic individuals. Without coverage, these families are likely to face more barriers to accessing quality care and may face significant negative health impacts as a result.
On top of this, the pandemic has negatively impacted families’ financial stability, which in turn has drastic implications for widening health disparities. As a result of job loss, financial shocks, and reduced income, a growing share of the population is struggling to afford nutritious food, access quality medical care, remain safe and stably housed, and pay for costs related to education—factors which serve as central determinants of health. As state moratoriums on evictions come to an end, an increase in the number of individuals experiencing homelessness and housing instability will leave more communities vulnerable to the virus, as well as vulnerable to long-term negative health outcomes.
Tenants of color are disproportionately impacted by evictions, and cities across the nation such as Boston, Los Angeles, and New York are preparing to see an increase in the rate of individuals experiencing homelessness among Black, Hispanic, and immigrant communities. Within this context, it is becoming more and more clear that addressing health disparities that stem from unequal social and economic conditions is of absolute necessity to fight and recover from COVID-19.
Research to improve health care delivery and expand health care access
The COVID-19 pandemic has already placed an indelible mark on nearly every aspect of the United States healthcare system. To deal with an unprecedented crisis, we need new research demonstrating what works to adapt our health care practices, programs, and policies to best respond to and recover from the pandemic as quickly and effectively as we can.
What are effective and equitable strategies to deliver quality health care given new constraints imposed by COVID-19?
Community health workers are frontline public health workers who are trusted members of the communities they serve. Better understanding how these workers can facilitate access to health, social, and community services in a pandemic setting may be a critical component in ameliorating the impact of COVID-19 on communities with specific health needs, such as Indigenous communities and other communities of color.
Additionally, in a time of social distancing, when many health care services are no longer provided in-person or in clinical settings, it is important to better understand how interventions such as telehealth can be used and adapted to meet the needs of different communities, especially those where health care access is limited.
How can health officials increase take-up of positive health behaviors?
The widespread adoption of positive health behaviors is necessary to minimize the spread of COVID-19. Researchers should work with public health authorities to identify ways to improve take-up of positive behaviors such as wearing a mask, avoiding unnecessary crowds, and, when it becomes possible, receiving the COVID-19 vaccine. Examples of interventions to increase take-up may include information campaigns, direct encouragement to take-up services, or increased access to free masks.
What can health care delivery organizations do to provide accessible and impactful mental health care?
In a period of increased social isolation, uncertainty, and financial stress, accessible and impactful mental health services are more critical than ever. Loneliness and social isolation are linked to poor health and mental health outcomes.
Due to the closure of clinics, provision of mental health services and counseling are more difficult for individuals to access, and for many, accessing counseling is cost-prohibitive. It is critical to have data on the efficacy of innovative strategies to deliver mental health care in this new context, including telehealth and app-based mental health services.
How can health officials address the unique health needs for those experiencing major barriers to health care, including those who are uninsured, incarcerated, or experiencing homelessness?
People without insurance in the United States often minimize their use of health care due to the high cost of seeking care, and may be hesitant to seek out critical COVID-19 testing or treatment. Further, individuals who are incarcerated and those experiencing homelessness represent two groups who are at high-risk of COVID-19 infection, lack access to adequate health care, and are unable to practice the positive health behaviors recommended to limit the spread of COVID-19.
Researchers should work with community agencies and health officials to identify effective ways to encourage the take up of health care for groups who largely lack access to care opportunities. Programs to broaden the reach of mental and physical health care service (such as mobile or telehealth platforms), increase trust in health systems and services, and connect individuals with social safety net programs may be important.
This post is an installation in J-PAL North America's "Building An Effective COVID-19 Response" research guide blog series. The complete series highlights the interaction between COVID-19, research, and the policy areas of health care delivery, jobs and the social safety net, and education.
Social distancing guidelines in Indonesia and around the world have profoundly impacted many aspects of people’s lives, from the way we communicate to the ways we work, shop, and transact. These shifts have brought the potential of digital financial services as a means of easing some of the economic consequences of the COVID-19 shock in Indonesia to the forefront.
Social distancing guidelines in Indonesia and around the world have profoundly impacted many aspects of people’s lives, from the way we communicate to the ways we work, shop, and transact. These shifts have brought the potential of digital financial services (DFS) as a means of easing some of the economic consequences of the COVID-19 shock in Indonesia to the forefront.
While anecdotal evidence suggests DFS adoption is on the rise nationwide, policymakers lack concrete evidence on how widespread adoption is and what new users’ experiences look like. To examine whether the pandemic has increased the use of DFS in Indonesia, J-PAL Southeast Asia’s Inclusive Financial Innovation Initiative (IFII) team collaborated with an Indonesian government partner to conduct an online survey on DFS adoption.
The survey was conducted through Google Surveys, which uses convenience sampling to recruit people through mobile phone and computer-based Google platforms. Accordingly, the sample is skewed towards people who are digitally engaged, often considered as an important target group for DFS conversion.
Increased DFS use during the pandemic
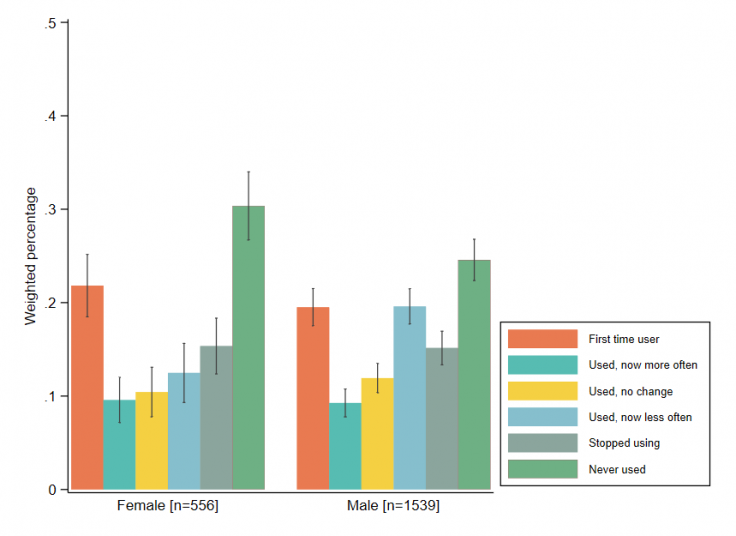
Notes: Results are weighted using SUSENAS 2019. The numbers in parentheses are sample sizes. Whiskers denote 95 percent confidence intervals.
Key findings
More people are using DFS during the pandemic. Twenty-one percent of men and 22 percent of women in the survey reported that they used DFS for the first time during COVID-19, while 15 percent of men and women reported that they stopped using DFS in this period.
As online platforms often offer discounts and shoppers can compare prices more easily than in physical stores, we found that the desire to find cheaper goods online is one of the biggest triggers of DFS adoption. Other drivers of use are the greater safety and convenience of online shopping, as well as the need to more easily transfer funds.
DFS users do not go fully digital. Sixty-two percent of DFS users use online platforms to buy primary goods like food and drinks, or secondary goods like clothing, books, stationary, and household utensils; however, 54 percent of online shoppers report cash is still their main payment instrument. The most common reported barriers for using electronic payment technologies like digital banking and e-money are a perceived lack of use cases, associated fees, and trust issues.
Promising signs of inclusion among harder-to-reach groups
J-PAL’s survey suggests that women and rural dwellers are actively adopting DFS during the pandemic; moreover, older Indonesians (45+) have a higher take-up than the younger population—at least within the highly-selected Google Survey sample.
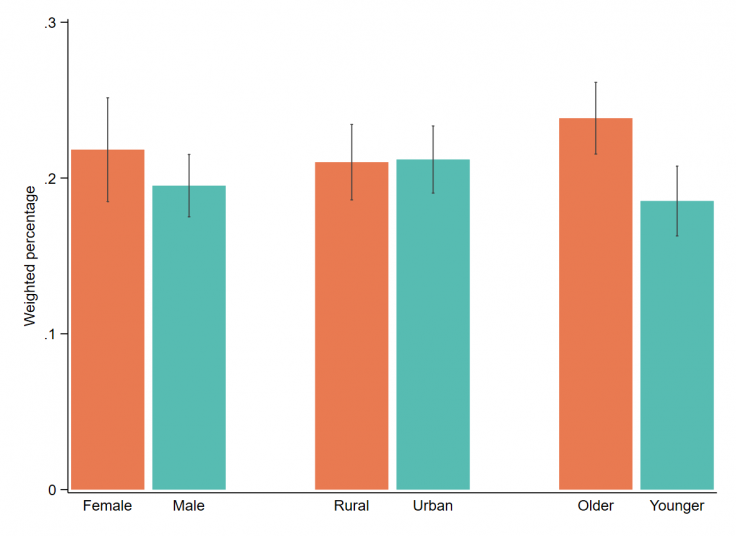
Notes: Results are weighted using SUSENAS 2019. Age category is split between the older group (45 and older) and the younger group (18 to 44 years old). Whiskers denote 95 percent confidence intervals.
Women and rural residents report being first-time DFS users at the same rate as men and urban dwellers, which is crucial to lift up who are more likely to be excluded from the financial system. Female DFS user are also more frequent online shoppers (84 percent of women versus 76 percent of men). Accordingly, online shopping could provide a compelling business case for women to adopt DFS after the pandemic abates.
Older individuals are more likely to convert to DFS. Twenty-four percent of people aged 45 and above are first time adopters, as compared to 19 percent of people aged 18 to 44. Part of this may reflect higher pre-pandemic use among younger individuals, who are often more digitally literate.
What can industry and policymakers do to support sustained DFS use among new adopters?
Pandemic-induced shifts in adoption are more likely to convert to meaningful longer-term engagement if new users have positive experiences early on.
Private sector players should pay attention to user onboarding and communication to ensure that getting started is easy. They could also ramp up promotion efforts by expanding incentives (discounts, cash-back, etc.) to create habitual DFS use. At the same time, government agencies could build on recent initiatives that leverage DFS for social protection payments.
Efforts now to help new users get comfortable and stay engaged may pay long-term dividends as Indonesians adjust to a “new normal” way of managing their finances and participating in the economy.
J-PAL Southeast Asia’s Inclusive Financial Innovation Initiative (IFII) is working alongside governments, private sector firms, and nonprofit organizations to understand how the COVID-19 pandemic has shaped the way people live and transact.
This blog post is based on effort funded by the Bill & Melinda Gates Foundation. The findings and conclusions contained within are those of the authors and do not necessarily reflect positions or policies of the Bill & Melinda Gates Foundation. The mission of IFII is to ensure that digital financial services can drive economic development while lifting up women, low-income groups, and marginalized communities.
You can review the detailed results of the online survey here. For more information about IFII, contact [email protected].

